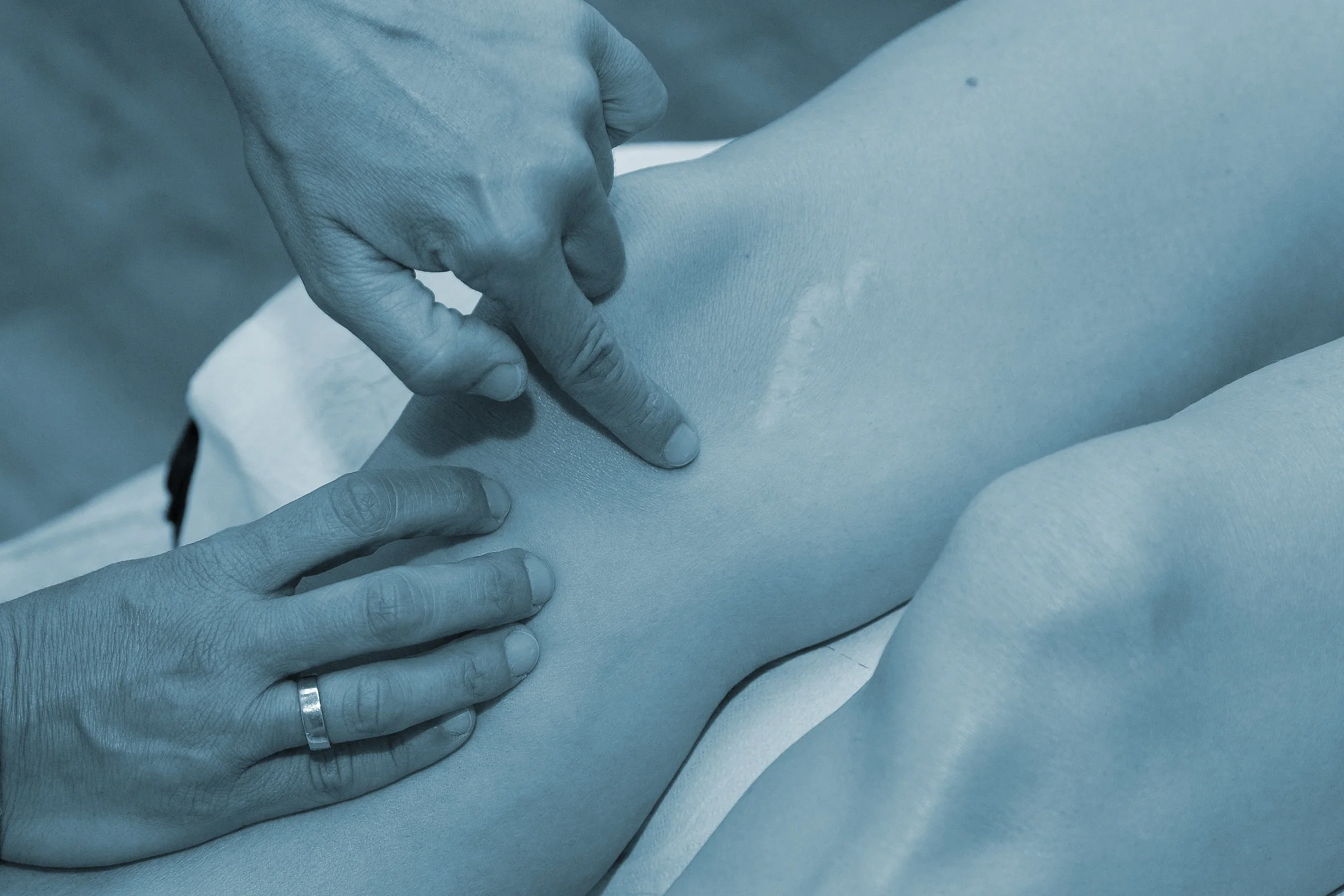
EDUCATIONAL RESOURCES
Evidence-based resources to help you understand, recover and move well.
Good information is part of good treatment.
We've always believed that leaving our clinic with a better understanding of your body is just as important as leaving with less pain. Over the years we've written about the things that come up again and again in the treatment room — the questions people ask, the myths worth busting, and the practical tools that actually make a difference between appointments. Some articles are grounded in the latest pain science, others are refreshingly simple. All of them are written by the people who treat you, for the people they treat. Have a read, bookmark what's useful, and bring your questions when you come in. Check our blog for more.
UNDERSTANDING PAIN
Pain is the main reason people walk through our door, and it turns out there's a lot worth knowing about it. The last twenty years have produced a remarkable shift in how we understand pain, away from the idea that it simply reflects damage in the body, and toward something far more interesting. The brain, the nervous system, your history, your stress levels, your sleep, your beliefs about what's wrong, all of it shapes the experience of pain in ways that matter enormously for how we treat it. Getting your head around this stuff isn't just interesting. It's genuinely useful.

WHAT’S RIGHT WITH ME
A colleague recently posted a link to a study that focused on spousal bereavement, or in layman’s terms, the feelings we experience when we lose a loved partner. There are multiple studies on the impact of health after the death of a partner and there is a resultant increase in GP visits for both physical and mental ailments (1).
-
With all those increased visits to the GP, there comes with it the potential for the GP themselves to feel helpless as a caring health practitioner. Having a sad and bereft person sitting in front of you may not be the regular focus of their practice and there are always time pressures involved. Hence the potential for patients being offered a ‘diagnosis’ of depression (2) and anti-depressants are prescribed as a relatively cheap intervention for people’s suffering. Albeit, with only a small benefit (3). Importantly, in this interaction, we need to acknowledge that most people visiting the GP don’t want to keep feeling the way they feel and are pleased with a label and a solution.
AND THE MORAL OF THE STORY IS?
My long-winded point is that we can be prone to pathologize* something that is completely, whilst unfortunate, normal. It is normal to feel anxious, sad, etc. and the question arises when does this cross over into something abnormal or into a ‘diagnosable’ condition? Perhaps the practitioner is relieved to give it a name, or equally, perhaps the patient is? Either way everyone’s intention is to ease suffering.
Over diagnosis and over prescription for depression is concerning, but what’s the link to pain?
PAIN IS NORMAL
Pain is normal. It might be irritating, confronting or downright awful but it’s infrequently insufferable. And on most days, pain is essential for our survival. It protects us from touching hot things that will burn us, it causes us to stop the flow of blood when we cut our finger, it makes us stop and rest when we’ve torn a ligament in our ankle and it stops us overloading to the point of heatstroke in an Ironman competition.
We are all at risk of pathologising something that is normal and it worries me when this message comes thick and fast from the medical voice of authority:
there is something (or everything) wrong with your posture
there is something wrong with your bones, ligaments, muscles, nerves, etc
there is something wrong with your desk, your shoes, your style etc.
there is something wrong with your running style, your swimming style, etc
there is something wrong with the food you eat, etc
there is something wrong with you!
And now, let’s fix that, with corrective exercises, corrective food, corrective supplements, corrective treatment (I know that’s my bit). There is a place for some of these things, we could all move more, eat better, sleep more, wear better shoes, be more mindful, hug more and take deeper breaths. But there is no getting away from the fact that pain is normal.
I’ll admit I’m as intolerant of pain as the next person. I’ll frequently reach for ibuprofen at the onset of a migraine or ask a colleague for a treatment when I have an aching low back. But I know that what I’m experiencing is normal. I listen to what the pain is trying to tell me (don’t drink red wine or lift mattresses by myself) and I take measures, where possible, to alleviate any predisposing factors.
SO LET'S FIND OUT WHAT'S RIGHT WITH YOU.
Disclaimer: there are times when pain isn’t normal and becomes the alarm bell that won’t stop ringing, and if all sinister reasons have been ruled out then we are left only with complex uncertainty, but that story is for another BLOG.
1. Charlton R, Sheahan K, Smith G, Campbell I. Spousal bereavement – implications for health. Fam Pract 2001;18:614–8.
2. Stroebe M, Henk S, Stroebe W. Health outcomes of bereavement. Lancet 2007;370:1960–73.
3. Kirsch I. (2009). The emperor’s new drugs: Exploding the antidepressant myth. London, UK: Bodley Head.
This is a link to the article that sparked this article:
http://www98.griffith.edu.au/dspace/bitstream/handle/10072/40154/70829_1.pdf?sequence=1
* Pathologize = to take some way of reacting, feeling, or being and to treat it as a disease.

Slow and Steady Wins the Race
When pain hangs around for longer than expected this can be immensely frustrating for patients. But when problems are complex and recalcitrant they can also be frustrating for practitioners and requires patience from both parties. If a patient has a story of brokenness, then it takes the right information, at the right time provided in the right way for that person to help turn that story into one of hope.
-
So many of us are pressed for time and aren't we all searching for the simple, immediate solution to any problem? Often a simple and effective solution can be manual therapy. Good practitioners can be really good at providing an immediate relief for pain. Whether it lasts is another story and the transient relief for patients can be at once addictive and ultimately frustrating.
A good practitioner will combine manual therapy and education. Education comes in multiple forms, knowledge about why it hurts, and information about pain can help redirect the assumption of brokenness. Education can also be advice about unhelpful behaviours, thoughts or beliefs. And it most certainly should involve having a discussion about the true the true nature of pain and what it means for your recovery.
A good clinician will help find your baseline for activities and armed with good knowledge, your brain and body will know you're safe even if you experience some discomfort.
A fair amount of frustration exists around trying to increase physical activity, which as we know from the literature (and the media) is a magic bullet (1). But many people have the experience that simply increasing the amount they move increases their pain. Often, they'll take the weekend warrior approach. They join a gym and do a body balance class and end up crawling in for pain relief as their low back and neck are screaming at them. If the alarm bells are ringing and you're getting negative feedback from every part of you it's hard to make the connection that it's a) good for you, and b) we need to do more of it and finally c) do it forever.
A good clinician will help find your baseline for activities and armed with good knowledge, your brain and body will know you're safe even if you experience some discomfort.
I listened recently to a great podcast with Neil Pearson, who is a physical therapist in Canada, who uses graded exposure to therapeutic yoga to help people with complex pain problems. But it doesn't have to be yoga that gets you there. The simple and free option is walking.
What is graded exposure?
Graded exposure is a fancy way of saying that you need to start with a small amount of something that threatens you and as your brain and body tolerate it, add in a bit more the next day until you can participate in an activity you enjoy without a backlash.
So what does a graded exposure program to walking look like?
Start with a baseline of 10 minutes per day at around 65% of your maximum heart rate. In the range of comfortably carrying on a conversation. Up the benefits and go with a friend.
You need to assess how you feel afterward. If you have any adverse effects, ask yourself, do they last five minutes, five hours or five days? Depending on the answer, you need to increase or decrease the amount of time and effort you are making with walking. As a guide, anything more than a three hour increase in discomfort means you're overdoing it. Remember though to pay attention to your response AFTER your walk, not during, as this is a better indicator of how irritable your body and brain is.
If you don't overdo it, you'll improve so rapidly that after only a week you'll want to start increasing the amount of time, slowly now, to get to the point where you can walk for 45-60 minutes. It might take eight weeks or it might take six months, depending on how your body responds.
When you reach the 60 minute range, you'll be improving brain health, fighting Alzheimers, etc, you'll definitely be burning fat, if that's your extra goal achieved.
When you can comfortably walk in this time range with no negative repercussions, you can add in some moderate intensity exercise, like a 30 second jog, and then another 30 second jog later in the walk around 75% of your maximum heart rate. Once you've worked up to 6 x one minute jogs, then you're ready to add in some additional activities that take your fancy.
Strength work, flexibility and high intensity exercise come after all this preparation. You'll be so much more connected to what your body might want to achieve and what you might enjoy. If you enjoy being out in the sunshine, then there are myriad options at your disposal. Do something you like, do it with a friend and do it for your mental health, as well as to improve your pain.
Nerves and Radicular Pain (ridiculous pain)
I used to think that nerves were microscopic. This was before I knuckled down to five years of study at University. Now I know that every part of the body has a nerve supply and you don’t need a microscope to see them. It all starts from our brain, moves onto our spinal cord and then nerves branch off and travel outward to EVERYTHING and when you put it all together it’s known as the nervous system.
-
The nervous system is super important
Potentially, I can’t overestimate the importance of the nervous system. We would be a gelatinous blob without it. It manages 100% of everything, 100% of the time and it’s hungry for oxygen and glucose and if it doesn’t get these things it sends danger signals to our brain very quickly so that we can do something about getting them what they need. Normally this will involve fairly basic tasks like moving, moving so we can get something to eat and moving so that we can go somewhere to lay our head and go to sleep.
The nervous system is super sensitive
The 72 kilometres of nerves in our body exist to relay signals/information from bits of our body to the brain or from our pink, squishy brain out to bits of our body. These wonderful information carriers are sensitive to everything; chemicals, touch, movement, they are constantly monitoring every little thing about us. A short distance away from where the nerve exits the spinal cord, there is a very sensitive part that if entrapped or irritated by specific chemicals this may cause increased activity of that nerve. Increased activity means the nerve sends off lots and lots of information to the spinal cord and brain, which you might detect as pain or altered sensation in the skin.
This is what is known as ‘radicular pain’ as it ‘radiates’ through the body, most likely into our arm or leg, along the pathway of a nerve that has exited the spinal cord at your neck or lower down in the spine.
People will present to the clinic with pain into the arm or leg that seems to follow a pathway down a specific area. Radicular pain can present differently for different people. It may be felt as numbness and tingling, or burning pain, or a sharp, jabbing pain, or electric-shock like pain or extreme sensitivity to touch. When a nerve that exits the spinal cord in the low back, commonly radicular pain will be a gnawing, constant pain in their bum.
Who gets radicular pain?
It is estimated that between 13-40% of people will experience radicular pain at some point in their lives. There is a link to age, with the highest number of cases occurring between 40-50 years of age, and genetics may predispose this condition (1).
Is it my job's fault?
Some jobs seem to contribute to the development of radicular pain, such as working in awkward positions where the body is bent or twisted, with your hands above shoulders or when driving for prolonged periods. Equally, sitting a lot is starting to gain momentum as a risk factor for all sorts of conditions, including radicular pain. Smoking also increases the risk of radicular pain, as it alters the metabolic balance within the tissues of the spine (1).
If I have it, what can I do about it?
Most patients with radicular pain experience some improvement within four weeks from the onset of pain (2). The majority of cases resolve spontaneously with a multi-modal approach of pain relief such as anti-inflammatories or opioid based medication (1) and other more conservative measures, like manual and physical therapy or pain education (3). A number of studies supports the theory that a combination of treatments can lead to better outcomes (i.e. less pain) after three months, when compared to patients receiving either medication or physical therapy alone (4).
Can’t you just inject it? Or cut something out?
A 2014 review of research on radicular pain recommends that patients try 4-8 weeks of conservative treatment, before seeking more invasive interventions like spinal injections or surgery (5). It may seem like a long time to wait, especially when pain may cause difficulty sleeping, or reduce our ability to concentrate or enjoy even the most simple things in life.
Osteopathic Intervention
Manual therapy techniques along with exercise based rehabilitation is at least as effective as surgery for radicular pain (5) without the negative side effects. It’s frustrating but learning about what is happening, knowing the prognosis and enjoying even brief episodes of relief can provide hope and keep people focused on the light at the end of the tunnel.
Your osteopath can provide further information on these options. Book online to make a appointment.
References
(1) Woods, B.I & Hilibrand, A.S. (2015). Cervical radiculopathy: epidemiology, etiology, diagnosis and treatment. Journal of Spinal Disorders & Techniques, 28(5), 251-259
(2) V. J., Lubelski, D., Steinmetz, M. P., Benzel, E. C., & Mroz, T. E. (2014). Optimal Duration of Conservative Management Prior to Surgery for Cervical and Lumbar Radiculopathy: A Literature Review. Global Spine Journal,4(4), 279–286.
(3) Clark, C.L., C.G. Ryan, et al (2011). “Pain neurophysiology education for the management of individuals with chronic low back pain: systematic review and meta-analysis.” Manual Therapy 16 (6): 544-549.
(4) Cohen, S.P., Hayek, S., Semenov, M.A., Pasquina, P.F., White, R.L., Veizi, E., Huang, J.H.Y., Kurihara, C., Zhao, Z. et al. (2014). Epidural steroid injections, conservative treatment, or combination treatment for cervical radicular pain: a multicentre, randomized, comparative-effectiveness study. Anesthesiology, 121, 1045-1055.
(5) Boyles, R., Toy, P., Mellon, J., Hayes, M., & Hammer, B. (2011). Effectiveness of manual physical therapy in the treatment of cervical radiculopathy: a systematic review. The Journal of Manual & Manipulative Therapy, 19(3), 135–142.
This article was a combined effort of Angie Bruce and Cat Burns. Angie was the one who admitted she thought nerves were invisible and Cat provided the bulk of the sensible information and academic references.
MOVEMENT AND MOBILISATION
Moving well is one of the best things you can do for a body in pain but it's also one of the first things to go when something hurts. The instinct to protect, guard and rest makes sense in the short term, but it has a habit of sticking around longer than it should. The good news is that getting movement back on board doesn't have to mean a gym membership or a gruelling exercise program. Sometimes it's as simple as knowing which movements to do, how many times, and with what attitude. Joyful, purposeful and pain-free is the goal. We've put a lot of thought into making that as accessible as possible.

Seated Rotations
Get Your Body Moving — 30 Mobilisations for Everybody
Let’s be honest people. We can’t always be as active as we want. We find it inconvenient and at times impossible to answer the call for natural movement*. It’s hard to run across the grassy plains when we’ve only got a concrete path or it takes a two-hour train ride to get to a wilderness trek up the side of a mountain. And we have to be dedicated in searching out opportunities to squat, throw something, wrestle, dance, run, leap, climb or hang upside down off a branch.
-
We need to do these things, but when we can’t, you can offer something else to your beautiful body. Something to nourish, so it can flourish! And so comes the concept of 30 ideas to mobilise your body.
WHAT THE HECK ARE MOBILISATIONS?
Mobilisations are like dynamic stretching. They sit somewhere in between rehab and lifting weights. It’s difficult to get any specific research to support this kind of movement but we can draw some conclusions based on evidence supporting early movement after surgery for hip and knee replacement (1) daily movement for acute low back pain rather than bed rest (2) safe movement following a car accident instead of a neck brace (3) and a long history of committed movement in multiple cultures (tai chi, qi gong, ceremonial dancing, prayer and worship).
We might even want to throw it out there that mobilisations might be useful for:
pain relief
early healing
micro breaks
preventing pain
preventing injury (I said maybe!!)
the dip in the couch
We can get attached to not moving. You know the feeling when you’ve succumbed to the dip in the couch or you’ve shaped your body to the back of your ‘ergonomic’ chair. Our bodies sometimes try to get us to move out of desperation before the thinking part of our brain even gets a say. We crack our neck, stretch our back over the back of the chair or twist forcefully to one side. Take charge of your runaway body and acknowledge that alarm bell for what it is.
Convert that animal instinct into something to nourish your cells in all your tissues, including your brain. Pump and stretch those clumping cells and provide them with the nutrition they need via blood supply using the mechanics of your own body. Help juice up your joints, tendons, skin, brain cells, muscles, nerves, ligaments, organs and move those tubes that string them all together.
we've put together 30 great ideas to inspire the modern human to combat physical stagnation.
The rules to follow:
easy and painless
lots of repetitions (i can do it i can do it i can do a little bit more) 25-75 repetitions (1-3) sets/day
joyful, fun, no protocol, no commitment beyond maybe a few days
if you’ve tried to make it easier and it still feels bad (or pointless) then STOP
Side Rainbow
Seated Glute Stretch
Bear Hugs
Cat and camel
Catch a Butterfly
Wag the Dog
Leg Swing V2
Shoulder Swings
Chest Openings
Stir the pot
Hip release - Katy Bowman Style
Chest Opening and Closing
Assisted Squats
Thread the needle
Hip Drops
Leg Swings
The Lawnmower
Bow and Arrow Standing
The Shovel
Forearm mobilisations
Standing Rotations
Arm Swings
Ankle Twirls
Thread the Needle V2
Lower Limb and Glutes
Do the Swim
Neck Mobilisation
Foot and Ankle Mobilisation
Disco Time
PRACTICAL PAIN MANAGEMENT

STANDING FIRM
Why it sometimes hurts to stand from sitting?
The sit-to-stand (STS) is a test used to measure lower-limb strength in older people or those with significant weakness (1). It is considered an easy, quick and fairly valid measure, which involves measuring the time taken to stand from a seated position a certain number of times, or recording the number of repetitions you can do in a given period (2).
-
The sit-to-stand (STS) is a test used to measure lower-limb strength in older people or those with significant weakness (1). It is considered an easy, quick and fairly valid measure, which involves measuring the time taken to stand from a seated position a certain number of times, or recording the number of repetitions you can do in a given period (2).
The findings of recent studies suggest performance in this test is influenced not just by factors associated with strength, but also balance and mobility, and a vast array of psychological factors (1).
BUT WHAT ABOUT WHEN SIT TO STAND HURTS?
Low back pain can reduce spine, hip and pelvic floor motion due to conscious or unconscious guarding associated with pain (3).
Multiple studies have shown there are changes in how energy is transferred between bone and soft tissue in the spine, pelvis, and legs associated with pain (4). And that inefficient energy flow or transfer then places more demand from everything. A cycle of back pain-altered biomechanics can start, creating more back pain. With all the changes in energy transfer and muscle power, everyday activities such as standing up from a sitting position can become difficult.
Muscle coordination, balance and mobility are affected, and psychological factors start to play in and effect our beliefs and so the cycle continues (1). Stopping the cycle can be easy. You just bypass your traditional route to standing and try something different altogether.
Try these simple tips. You may not need all of them:
RELAX before you start
WIDER STANCE - think SUMO wrestler
SLOW DOWN (TIMING) - move more slowly
HANDS ON KNEES
BREATHE OUT - this is a big one. The less compression in the container of the torso the better.
Many people are surprised they can suddenly sit-to-stand with no pain after weeks or months experiencing twinges and outright muscle spasms when trying to stand after sitting.
After a few days of pain free sit-to-stand, you can try heading back to your old ways as there is rarely a “right” way to do something. You can get up and down any way you choose, each one of them equally valid.
As a lot of research shows, the way you do something does start to matter. If you always get up and down via your arm on the desk, leaning forward to create momentum, it means the strengths necessary to do it another way are waning.
CAN THIS HELP IF I HAVE PAIN ELSEWHEREE?
This can also break the cycle if you experience pain in hips, knees and feet.
References
1. J Gerontol A Biol Sci Med Sci. 2002 Aug;57(8):M539-43. Sit-to-stand performance depends on sensation, speed, balance, and psychological status in addition to strength in older people. Lord SR1, Murray SM, Chapman K, Munro B, Tiedemann A.2. Exp Gerontol. 2018 Oct 2;112:38-43. doi: 10.1016/j.exger.2018.08.006. Epub 2018 Sep 1. The sit-to-stand muscle power test: An easy, inexpensive and portable procedure to assess muscle power in older people. Alcazar J1, Losa-Reyna J2, Rodriguez-Lopez C1, Alfaro-Acha A3, Rodriguez-Mañas L4, Ara I1, García-García FJ5, Alegre LM6.
3. Explain Pain Supercharged G. Lorimer Moseley and David S.
Butler. Adelaide City West: NOI Group Publishers, 2017. ISBN: 978-0-6480227-0-14. Gary L. Shum, PhD, et al. Energy Transfer Across the Lumbosacral and Lower-Extremity Joints in Patients with Low Back Pain During Sit-to-Stand. In Archives of Physical Medicine and Rehabilitation. January 2009. Vol. 90. No. 1. Pp. 127-135.

Is that a knot in my muscle?
54 year old Barbara has pain extending across the top of the shoulders, frequently extending into the neck. Is it a muscle? Is it a trapped nerve? Or is there something more complex going on? Why didn’t it hurt six months ago?
Surely, the muscles are tight?
-
They may actually be a bit wound up actually, especially with a little bit of stress in your life. Most of us have experienced a rush of adrenaline in the work place, at home or even crossing the road. Adrenaline is great; it prepares your body to get moving by increasing your heart rate and your breathing so you can send more oxygen to your muscles. The free-floating adrenaline also binds to your muscle spindles, increasing the resting tension so your muscles can burst into action.
Most of the time though, we’re left not bursting into action but taking a deep breath and getting on with not moving.
BUT IS ALL THAT TENSION GOING TO MAKE A KNOT?
One study specifically found there is no clear evidence of a strong relationship between increased electrical activity of muscles and the development of musculoskeletal disorders (2). Keep in mind this was one study, and the definition of a musculoskeletal disorder might not include Barbara and her sore muscles across the top of her shoulders.
I CAN DEFINITELY FEEL A KNOT IN THERE
There is zero consensus about what that hard lump in the muscle actually is and ‘knot’ seems like a fairly innocuous word to all those other than knitters and sailors. And just like knots in the real world, most are amenable to unwinding given the right intervention.
Bio (Body) Psycho (Brain) Social (Environment/Interaction)
Like many things in the body and pain, the pathophysiological mechanisms remain unclear. We are always more than the sum of our parts and if we look at the risk factors above, you need to find out whether Barbara has stress in the workplace, disappointment in her job, her relationship, whether she has a cold, whether her dog just died and she’s stopped walking, whether her children left her with five grandchildren on the weekend? And then what is her ability to control any or all of these aspects of her professional and personal life?
See the problem? This is why a medical history is important, why Osteopaths ask a lot of questions, why we need to spend more than seven minutes with you to grasp how to help you out of pain. We need to find out what’s tipped you from not even noticing that you’re a bit tight, to not being able to tolerate your shoulder discomfort a moment longer.
Hopefully, it’s as simple as softening off the muscles, turning a computer to a better angle, taking some micro breaks in the workplace and heading out for a daily walk.
Let’s get back to Barbara...
Step One: take a slow deep breath —drop your shoulders—release the tension
Step Two: Get up from your desk occasionally. Wave your arms around or run them quickly on the spot for ten seconds (Smile at your colleagues and let them know you’re not crazy).
Step Three: Find some daily exercise that you love
Step Four: Advise your children you can no longer care for all five grandchildren at once for an entire weekend.
References:
Ratey, John J.,Hagerman, Eric. (2008) Spark :the revolutionary new science of exercise and the brain. New York : Little, Brown,
Westad C, Westgaard RH, De Luca CJ. J Physiol. 2003 Oct 15;552(Pt 2):645-56. Motor unit recruitment and derecruitment induced by brief increase in contraction amplitude of the human trapezius muscle.

Jaws - The Curse of TMD
It has been over 40 years since the legendary movie "Jaws" was released. It was a cinema masterpiece of its time with bucket loads of suspense and horror that managed to scare everyone from swimming in the ocean for years afterward. With the clever use of animatronics, images of bloody big dorsal fins and spooky music it left movie goers nursing tense and sore jaws from clenching their teeth through anxiety and fear. Segue complete. See that? Jaws and jaw pain?
-
Jaw pain is a pretty common issue affecting 33% of the general population at some time in life (1). Of that population there seems to be more significant spike in the age range of 20-40 year olds, with a significant portion of that number needing to seek treatment from a health professional. Anxiety is a key contributor to jaw pain but it is not the only reason people experience pain in/around the jaw or temporomandibular joint (TMJ). We commonly refer to pain around the TMJ as Temporomandibular Joint Disorder or TMD. It is actually not one single disorder but representative of multiple sub groups of issues. They are typically categorised as muscle problems or joint problems.
WHAT CAN YOUR OSTEOPATH DO?
At Fairfield Osteopathic Clinic we take into account the whole person when dealing with the treatment of TMD. In other words we need to understand the underlying causal factors, which may range from mechanical joint factors, emotional stress or functional overuse issues (think Australian gum-chewing cricketer). There are also direct links between neck pain and TMD and any assessment will recognise the connection. There is plenty of evidence both clinically and through peer reviewed research to suggest that the neck and jaw are pretty tight in their relationship with one another (pardon the pun). One paper suggesting that 70% of TMD sufferers also experience neck pain (2).
A worthy TMD assessment will always encompass an actual physical assessment of the muscles around the jaw and the joint movement itself. This will guide treatment options. As osteopaths we use lots of direct and indirect techniques to modulate pain, but without addressing underlying causal factors that impact the jaw then relief may not last for long. These irritating causal factors might include chewing gum, chewing meals on one side of the mouth, specific dental issues, night time bruxism or teeth grinding and habitual jaw clenching (a lot of people don't realise they clench until they actively relax their jaw muscles). There are simple relaxation exercises for the jaw that are easy to practice and master. Head down to the end of the BLOG for some ideas.
SELF MANAGEMENT
Self management strategies are essential in dealing with any long term TMD. A large study published in November 2016 attempted to collate as much data on self management strategies and form a best practice management strategy for longterm TMD. These strategies include:
1. Education - a bit of positivity is a good start as pain is usually self-limiting. Understanding the anatomy and usual function of the TMJ complex and associated musculature can be helpful too. Other ideas include improved sleep hygiene (don't watch Jaws before bed), sensible and time-limited use of analgesia, avoidance of OTC splints bought without consultation with a dentist, limit caffeine usage, ‘doctor shopping’ won't help.
2. Self exercise therapy - gentle stretches for the jaw muscles and relaxation exercises, which are best explained by your osteopath.
3. Heat treatment - usually heat for sore jaw muscles is best. Ice treatment is best avoided due to the sensitivity of the nerves that innervate the area (remember ice-cream headaches)
4. Self massage therapy - there are very simple self massage techniques for the main jaw muscles and upper neck muscles. Again these are best explained in person as a little goes a long way.
5. Diet and Nutrition - it's important to establish a pain-free diet for at least three weeks. That means avoiding excessive chewing or hard-to-chew foods. In other words TMD sufferers may need to establish a "soft diet" until sensitivity decreases.
6. Parafunctional behaviour - this is the tricky one. There are often habits that irritate the jaw that we seem to not have as much control over e.g. grinding teeth or jaw clenching during sleep, which is called nocturnal bruxism. This may require some other modalities of therapy or medication to help. Reflecting on coping strategies for stress and anxiety may be pivotal to changing some of these nocturnal habits (3).
EASY EXERCISE
Stand in front of a mirror.
Hold your palms gently on the side of your face - covering your cheeks.
Let your lower jaw fall into your hands. In other words relax it and let it go all loose.
Now practice that again without using yours hands on your face. Make as long a face as possible.
If you are having trouble mouth the sound "Bah". It lets your lower jaw fall open. Repeat that until you get a sense of your jaw relaxing.
If you practice this in the mirror then when you are at work throughout the day you can put your hands on your face and use that as a trigger for your face and jaw to relax. You are creating awareness around the difference between tension and ease.
Good luck and don't hesitate to make a booking to see us if things are a bit out of control.
References
1. Wright, Edward F., and Sarah L. North. "Management and treatment of temporomandibular disorders: a clinical perspective." Journal of Manual & Manipulative Therapy 17.4 (2009): 247-254.
2. Silveira, A., et al. "Jaw dysfunction is associated with neck disability and muscle tenderness in subjects with and without chronic temporomandibular disorders." BioMed research international 2015 (2015).
3. Durham, Justin, et al. "Self‐management programmes in temporomandibular disorders: results from an international Delphi process." Journal of Oral Rehabilitation 43.12 (2016): 929-936.
WOMEN’S HEALTH
Women's bodies are extraordinary and complicated, and the healthcare system doesn't always do them justice. From the menstrual cycle through to pregnancy, postpartum recovery and menopause — and all the hormonal complexity in between — there's a lot going on that deserves more than a rushed appointment and a pamphlet. We've written about some of it here, and we treat all of it in the clinic.

SURVIVING BREASTFEEDING
I saw a lovely new mother yesterday who asked me “So how exactly do you survive this breastfeeding palaver?”
Aside from the obligatory tender nipples and general exhaustion, her experience of pushing a baby out, her subsequent recovery and breastfeeding on the whole had been positive. Her comment on the downside of breastfeeding was, ‘…there is just so bloody much of it’.
When you’re in the midst of the first few weeks, it’s hard to foresee that the frequency of feeds in the early weeks doesn’t continue forever.
What is rarely acknowledged is the additional stress on every new mother’s body, especially if things are going well. All that sitting, holding, squeezing, loving, staring, and connecting constantly to a needy, small human attached to your breast, can mean your neck, shoulders, arms and wrists can take a bit of a battering.
I asked this lovely mother to demonstrate some of the mobilisations she was doing to combat these behaviours.
Neck mobilisations when feeding
Bear Hugs
Bow and Arrow
Do mobilisations help?
They certainly won't hurt and they'll remind you to commit just a small amount of moving and thinking time to your own body every day.
I'm still feeling a bit broken.
Sometimes you need a helping hand to maintain the energy needed to nurture new humans. The osteopaths or massage therapists at Fairfield Osteopathic Clinic can work with you to manage any post-pregnancy, post-labour, excessive baby-carrying, or breast feeding aches and pains. You can book online or call 03 9489 0981 to schedule an appointment.

KEEPING ABREAST OF YOUR BREASTS
At the mature age of 42 I’m long past worrying about how small my breasts are and how much padding I need to stuff in my bra if I want to wear a low cut top. And now the days of breastfeeding are over, my breasts are just another part of my body heading south.
-
I haven’t always been so ambivalent. I undertook my Master’s research on the potential impact of bras on breasts. There were no significant findings from our very small pilot study. And more significant research shows that wearing a bra is not a risk factor for breast cancer (yes - even underwire) (1). Like all good myths though, it doesn’t stop nearly 20% of women surveyed on this topic thinking they are harmful (2).
I think many women, once they’ve relinquished the vanity about what they think their breasts should provide for them, get on with the job of ignoring them. And that’s what I like about the Jane McGrath Foundation and what they’re trying to do with the pink QV cream. Make checking our breasts part of our hygiene routine and we might be inspired to play our part in preventative health.
Of course, whilst the cream is a good reminder to check and is also a lovely bit of advertising for breast cancer awareness month, you can most certainly check your breasts without the pretty cream.
WHAT ARE THE MCGRATH FOUNDATION TRYING TO DO?
I applaud the McGrath Foundation’s serious attempt at some foundational research investigating whether women are breast aware. They surveyed a cross section of 1,288 women to determine if women knew the risk factors for breast cancer, and how often and how confident they might be in examining their own breasts and detecting any changes that might be present.
WHAT ARE THE RISK FACTORS FOR BREAST CANCER?
The study reports there are six proven risk factors for developing breast cancer (there might be more but no one has done a study on every potential risk factor).
• Strong family history of breast cancer (however, according to Cancer Australia’s Recommendations for the management of early breast cancer in women with an identified BRCA1 or BRCA2 gene mutation or at high risk of a gene mutation, only around 5-10% of breast cancers are due to hereditary / genetic mutations) (2)
• Being a woman
• Being a smoker
• Growing older
• Drinking alcohol
• Starting menstruation earlier or menopause later
The one that I certainly didn’t know about was starting menstruation earlier or menopause later. The role of hormones in breast cancer is a complex one and the study notes that there was a lot of confusion from survey respondents.
A seventh risk factor, taking the contraceptive pill, was identified. Considering the role of hormones just mentioned, I think many younger women feel concerned. The recommendations are not clear on this topic, however, there may be an increased risk while a woman is taking the contraceptive pill depending the dose (3).
WHAT ARE SOME INCORRECTLY IDENTIFIED RISK FACTORS?
In other words what do we think will give us breast cancer but actually won’t. Things like sunbathing topless, having breast implants or reductions and sleeping in a bra do not increase our risk of developing breast cancer.
The study also showed women who consider themselves breast aware were more likely to identify the myths as risk factors. Questioning our intuition is always a good move.
DO WOMEN SELF EXAMINE?
Being armed with the correct knowledge is a great start but are women, even those identified at risk, self-examining their breasts? And do they feel confident that they could detect any changes?
Without breaking down what this sample of women actually undertake, a summary of this questions sums up the predicament:
“Approximately one third of those who don’t check their breasts regularly say that this is because it has never occurred to them to do so. One in five indicate that they don’t know how to, or they forget.”
And hence the problem. Do we need to change our behaviour? The study found that even having a friend or relation who has been diagnosed with cancer doesn’t improve our vigilance. Interestingly, having daughters makes us more likely to self-examine.
HEALTH BEHAVIOUR CHANGE
Health behaviour change has become an entire industry, in both private and public sectors. From an individual to an entire population it’s a big job.
Multiple studies look at teaching skills-based interventions combined with goal setting to improve health behaviours as an adult.
A PhD study looked specifically at educating 9th grade girls on a self breast-examination combined with goal setting as a preventative health tool. The rational is that the knowledge and skill base will be present as they age, and combined with a knowledge of the risk factors, they may even implement their skills. The study noted there was excellent compliance over the time of the study, however, the novel interest in breast self-examination may wane over time.
WHAT EXACTLY SHOULD WE BE DOING?
The next article reviews what the research and the experts conclude about breast examination, whether we should be doing them and some handy advice on how and when to complete one if you want to and importantly, how to track your efforts.
REFERENCES
(1) GETTING A GRIP: A Report into Breast Health Understanding Among Australian Women in Australia (October 2016)
(2) Getting Youth to Check it Out!®: A New Approach to Teaching Self-screening Resa M. Jones, MPH, PhD; Ian J. Wallace, PhD; Alice Westerberg, BA; Kristyn N. Hoy, MPH; John M. Quillin, MPH, PhD; Steven J. Danish, PhD Am J Health Behav.TM 2015;39(2):197-203
(3) Recent Oral Contraceptive Use by Formulation and Breast Cancer Risk among Women 20 to 49 Years of Age Elisabeth F. Beaber, Diana S.M. Buist, William E. Barlow, Kathleen E. Malone, Susan D. Reed and Christopher I. Li DOI: 10.1158/0008-5472.CAN-13-3400 Published 1 August 2014
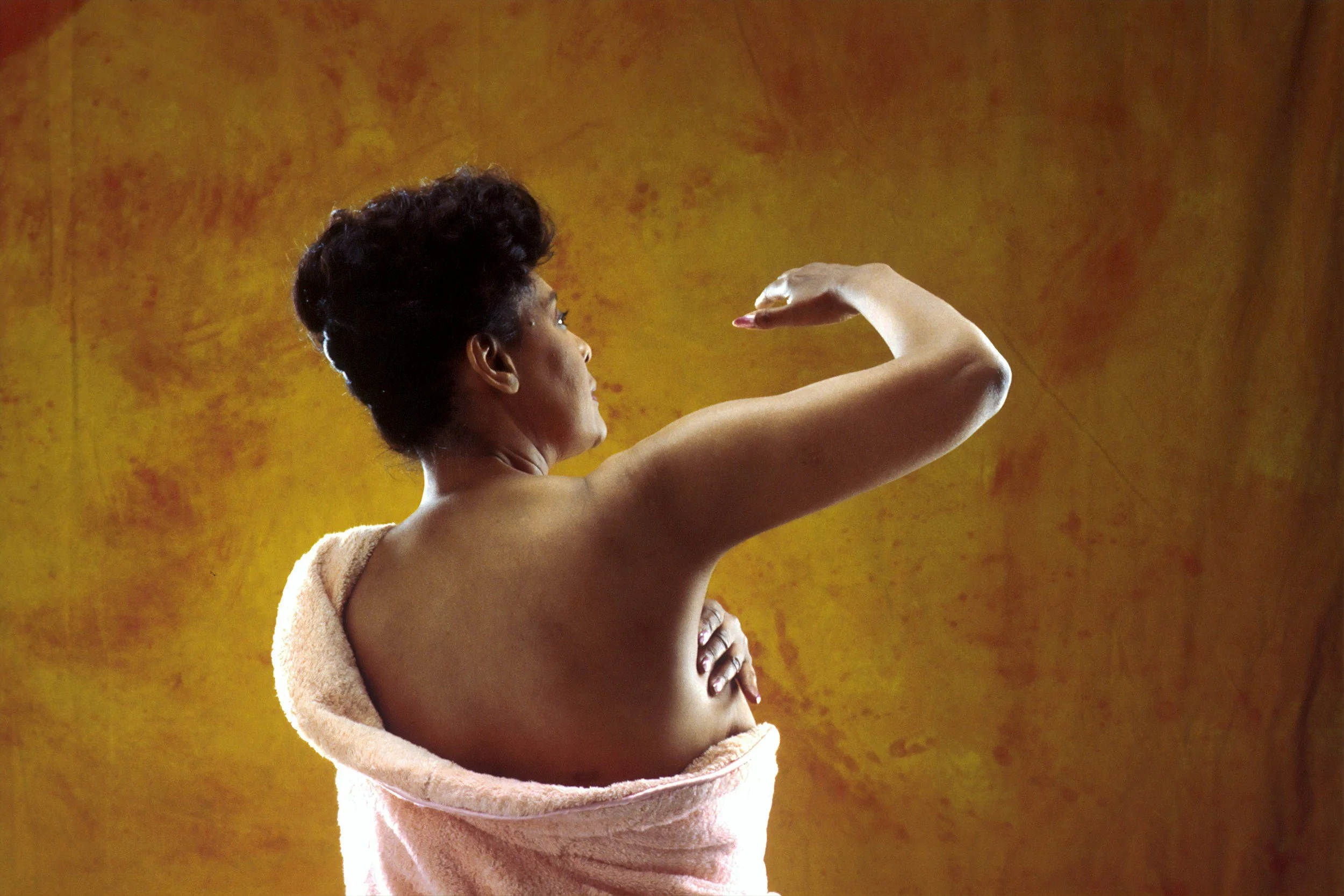
SHOULD WE BE PERFORMING SELF BREAST EXAMINATIONS?
Like many things to do with health and the human body, the evidence is muddy.
An opinion article published in the Journal of Obstetrics and Gynaecology of Canada (1) recommends that breast self examination should not routinely be taught to women as they concluded there were risks of unnecessary biopsies being performed with no reduction in mortality rates. They drew their conclusions largely due to a gigantic randomised, longitudinal trial completed in Shanghai (2).
-
WOMEN SHOULD COMPLETE BREAST SELF-EXAMINATION
There is less robust evidence that supports breast self-examination. It suggests excellent physical examination practice, whether breast examination performed by a health professional or breast self-examination, may reduce mortality (3).
I’m firmly in the camp of giving breast self examination a red hot go. You might feel things but not know what they are and whether it’s normal but like all skills, the more you examine your breasts, the better you’ll get to know them and find any changes.
IS THERE A PERFECT WAY TO DO A BREAST EXAMINATION?
Probably not.
GET TO KNOW YOUR OWN BREASTS
What is important is to know the look and feel of your breasts’ various peculiarities. Has that blobby area changed from a few months ago? Does something stand out as different from the rest (like a rock on a sandy beach)?
A 2005 systematic review suggests women should look and feel their breasts and know what is normal. They should also know what changes to look for and know what to do if a change is found (4).
This is a step by step taken from the USA breastcancer.org site, which is about as simple and as complex as you probably need to be.
YOU’LL NEED A MIRROR
STEP ONE: Look at the shape and appearance of your breasts and nipples in the mirror with your hands on your hips
STEP TWO: Raise your arms above your head and look at your breasts. Look for any changes in the shape of the breasts.
STEP THREE: Look at your nipples to see whether there is any fluid coming out.
STEP FOUR: Feel for lumps in the breasts either standing up or lying down.
STEP FIVE: Feel for lumps in the nipple area and in the armpits (5)
WHAT CHANGES AM I LOOKING FOR?
Armed with some knowledge of what is normal for you, detecting changes should be easier.
You’re on the lookout for:
New lumps
Thickening in breast tissue
Nipple sores
Nipple discharge
Nipples turning in
Skin dimpling
Rash
Red swollen breasts (6)
If you notice any changes report to a health professional IN A TIMELY MANNER. Rushing off every month will probably leave you and your GP frustrated. Equally, don’t wait just because you don’t want to bother anybody with your weeping, red nipple.
HOW OFTEN DO I NEED TO CHECK MY OWN BREASTS?
Tricky. A slow progression may not be noticed if you undertake an examination every month. However, if you don’t complete it often enough then you won’t know what normal is.
An educated guess would be four times a year?
WHEN TO COMPLETE?
Choose a day that's easy to remember, such as the first or last day of the season. If you are still having your period, complete the check a few days after your period has ended.
SHOULD I KEEP RECORDS?
Many people find keeping records onerous and it might stop you from even peering at your boobs in the mirror. Another person might find it essential to set an alarm, and keep thorough notes on their phone.
WE SHOULD BE MORE CONFIDENT TO CHECK
Learning how to undertake a breast self-exam is the first step as we spend far more time with our breasts than anybody else.
IF YOU’RE 50+
BreastScreen Victoria provides free mammograms to women over 50 as over 50% of women diagnosed with breast cancer are 50-69.
References
(1) Journal Obstetrics and Gynaecology of Canada 2006; 28(8):728–730
(2) Thomas DB, Gao DL, Self SG, Allison CJ, Tao Y, Mahloch J, et al. Randomized trial of breast self-examination in Shanghai: methodology and preliminary results. J Natl Cancer Inst 1997;89:355–65
(3) Harris R, Kinsinger LS. Routinely teaching breast self-examination is dead. What does this mean? J Natl Cancer Inst 2002;94(19):1420–1.
(4) McCready, Littlewood, Jenkinson. Breast self examination and breast awareness: a literature review. Journal of Clinical Nursing 2005 (14); 570-8.
(5) http://www.breastcancer.org/symptoms/testing/types/self_exam/bse_steps
(6) GETTING A GRIP A Report Into Breast Health Understanding Among Women In Australia Based on independent research carried out by AMR for the McGrath Foundation October 2016
MEN’S HEALTH
Men are not great at asking for help. This isn't a character flaw, it's a pattern deeply embedded in how masculinity has traditionally been defined, and it has real consequences. Men die on average four and a half years earlier than women, are significantly more likely to die by suicide, less likely to see a GP, and more likely to present to healthcare late, when conditions are harder to treat. The tide is shifting slowly, with initiatives like Movember and RUOK doing important work to open up the conversation. But there's still a significant gap between what men are experiencing and what they're prepared to talk about. We'd like to help close it a little.

BRIDGING THE GAP TO BETTER HEALTH FOR MEN
Every Movember Men's Health is in the spotlight. In particular Mental Health, Prostate Cancer and Testicular Cancer. Three aspects of Men's Health that contribute significantly to men's mortality. The saddest part of this statistic is that they are, to a great extent, preventable causes of death with early intervention.
In the course of my career I have taken many a phone call from the wife or partner of a man to make a booking on their behalf. Often unbeknownst to the man! This gives a small insight into men's health behaviour that is quite curious. Men will often avoid seeking attention for health related issues.
-
Why don't men ask for health help?
A study from the International Journal of Consumer Behaviours (1) found some interesting reasons why men do not seek health care assistance when they clearly should. These were broken down into broad themes that included:
Health-seeking behaviour was seen as a more female trait and not one associated with male self-reliance (I think this might be code for "I'm too scared to find out what's wrong with me")
Expressions of underlying fear and fatalism (at least they're being honest!)
Feelings of disconnection from health providers (talking about how I feel with a stranger is just not cool)
There is no good age to be a man
At the pointy end, the life expectancy of a man is on average 4.5 years less than a woman.
Perhaps more alarming, across the lifespan, just being a man means you're more likely to die than a woman. And that's in all major age groups! This is in part due to men being biologically driven to partake in more risky behaviour (with sometimes devastating consequences). However the stark difference across the lifespan points more directly at men's lack of attention to detail in maintaining their own health and well-being (2).
Health behaviour change and the time it takes
One of the major benefits of seeing an osteopath at Fairfield Osteopathic Clinic is the time we take with our patients. An initial consultation is usually around one hour and all subsequent consults are around 30mins. There is always opportunity to get to know the patient in front of us. Of course we'll take a detailed medical history and perform the appropriate physical examination. But more than that it is chatting to the patient about their life, family, work, hobbies, exercise routine, friendships - all the stuff that makes them who they are. Obviously this doesn't all happen in one consultation, it will often take a while to build a therapeutic relationship with a patient and trust is not something that can be afforded lightly. Often this chat can reveal something about them that needs a little more attention. This might work a little better with men who are more reserved about revealing too much about their health history.
So a shout out to the men out there. Don't put that appointment off with the osteopath because you think that it's not "manly" to see someone about your aches and pains. This goes double for those things that you should see the GP about e.g. a spot that has changed on your skin, a lump that has developed somewhere it shouldn't, or you just aren't feeling your "manly" self.
Taking ownership of your health
Influencing health behaviours is usually a pretty subtle science, even as a health professional. In recent times initiatives like Movember have done terrific work in highlighting the need for men to take ownership of their health. Likewise the RUOK group have done great work in clearing the lines of communication to help men (and women) open up about struggles with mental health. Always keep in mind that your health professional is a confidential source for anyone to talk about their health problems. As osteopaths we always are aware of our professional boundaries and scope of practice and will refer you on as necessary.
(1) Buckley, Joan, and Seamus Ó Tuama. "‘I send the wife to the doctor’–Men's behaviour as health consumers." International Journal of Consumer Studies 34.5 (2010): 587-595.
(2)http://www.ausstats.abs.gov.au/ausstats/subscriber.nsf/LookupAttach/4102.0Publication30.06.104/$File/41020_MensHealth.pdf